 
Since neither inspiratory push nor expiratory pull is effective in such an open circuit, HFNC cannot actively enhance V T. While interfaces for NIV increase anatomical dead space, those for HFNC actually decrease dead space. Another major difference between NIV and HFNC is the interface. The gas is heated and humidified with the active humidifier and delivered through the heated circuit (Figure 1). At the air/oxygen blender, the inspiratory fraction of oxygen (F IO 2) is set from 0.21 to 1.0 in a flow of up to 60 L/min. The apparatus comprises an air/oxygen blender, an active heated humidifier, a single heated circuit, and a nasal cannula. High-flow nasal cannula (HFNC) oxygen delivery has been gaining attention as an alternative means of respiratory support for critically ill patients. Because of poor mask tolerance, however, NIV is sometimes inapplicable. For patients with acute exacerbation of chronic obstructive lung disease (COPD), noninvasive ventilation (NIV) has become the preferred primary modality for respiratory support because it enhances inspiratory tidal volume (V T) and maintains adequate alveolar ventilation. Currently, to ensure adequate alveolar ventilation, minute ventilation is manipulated during invasive or noninvasive ventilatory support. In this, ensuring adequate alveolar ventilation is essential for expelling carbon dioxide produced in the human body. The purpose of respiratory support is to maintain adequate ventilation and oxygenation. Despite these issues, HFNC oxygen therapy is an innovative and effective modality for the early treatment of adults with respiratory failure with diverse underlying diseases. Some important issues remain to be resolved, such as its indication, timing of starting and stopping HFNC, and escalating treatment. Many published reports suggest that HFNC decreases breathing frequency and work of breathing and reduces needs of escalation of respiratory support in patients with diverse underlying diseases. Evidence with critically ill adults are poor however, physicians apply it to a variety of patients with diverse underlying diseases: hypoxemic respiratory failure, acute exacerbation of chronic obstructive pulmonary disease, post-extubation, pre-intubation oxygenation, sleep apnea, acute heart failure, patients with do-not-intubate order, and so on. Most of the available data has been published in the neonatal field. While there have been no big randomized clinical trials, it has been gaining attention as an innovative respiratory support for critically ill patients. It delivers adequately heated and humidified medical gas at up to 60 L/min of flow and is considered to have a number of physiological effects: reduction of anatomical dead space, PEEP effect, constant fraction of inspired oxygen, and good humidification. Conclusion: The use of HFNC oxygen therapy in infants hospitalized with acute bronchiolitis reduces PICU and hospital stay as well as the potential complications which will substantially reduce the hospital cost.High-flow nasal cannula (HFNC) oxygen therapy comprises an air/oxygen blender, an active humidifier, a single heated circuit, and a nasal cannula. The most common adverse event during the hospital course was respiratory failure which was seen among 4 patients in non-HFNC group and none among HFNC group developed such complication. There was early and better improvement in SPO2 and respiratory rate (p<0.001), decreased length of hospital stay (p<0.001) and PICU stay (p<0.01) among the patients in HFNC group as compared to non-HFNC group. Results: Out of 100 patients studied, 50 received HFNC oxygen and 50 received conventional oxygen. 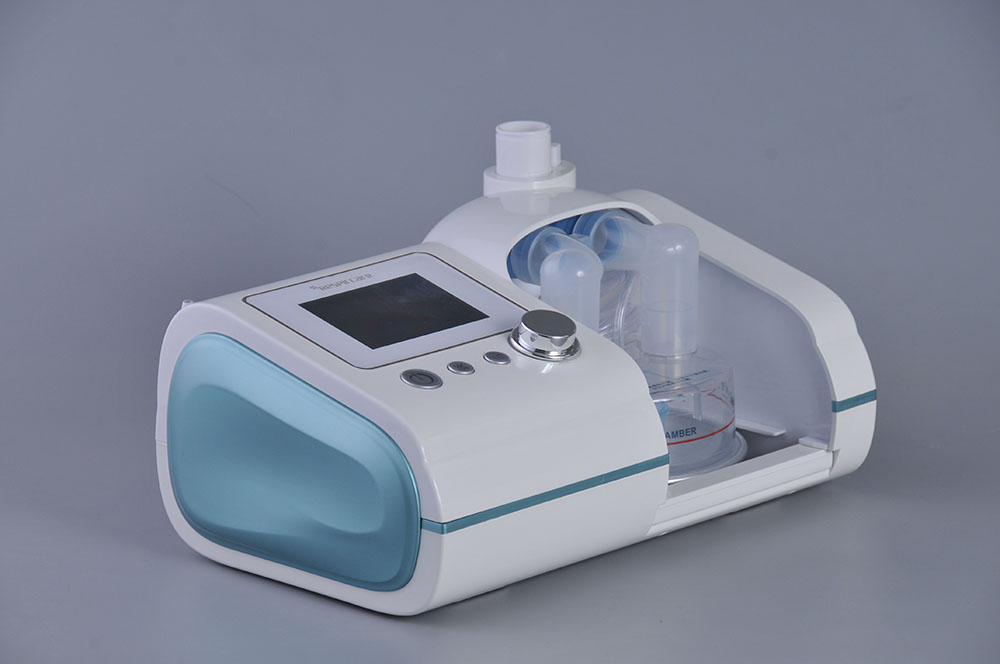
Outcome parameters measured were duration of hospital stay, duration of pediatric intensive care unit (PICU) stay, oxygen saturation (SPO2), respiratory rate, adverse event (respiratory failure), need for intermittent positive pressure ventilation or continuous positive airway pressure. The patients were randomized in each arm by simple randomization. The patients were divided into two groups: Patients in Group 1 received HFNC oxygen therapy (HFNC group) while those in Group 2 received conventional oxygen therapy (non-HFNC group). Methods: All previously healthy children between 1 and 24 months of age with an established clinical diagnosis of moderate to severe bronchiolitis (clinical severity score ?4) were enrolled for study. However, the latest studies have revealed that oxygen therapy via heated, humidified, high flow nasal cannula (HFNC) allows the delivery of high inspired gas flows which is better than the traditional one. 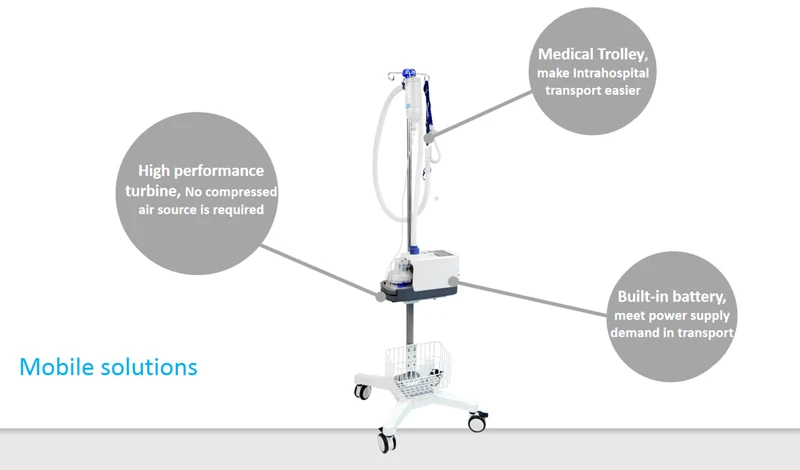
Traditionally dry oxygen is provided at 100% concentration via low flow nasal prongs. Bronchiolitis, High flow oxygen, Hospital stay, Infants Abstractīackground: Bronchiolitis is a major cause of morbidity and leading cause of hospitalization, mostly in early childhood without coexisting illnesses. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
